This week, we mourn the passing of Robin Williams, the brilliant comedian we counted on to lift our spirits, whose life tragically ended with Mondays suicide. Robin Williams is neither the first nor the last to commit this hopeless act. Over 38,000 individuals complete suicide in the United States annually. This translates to one completed suicide every 15 minutes and over 100 suicides daily. In fact, suicide is the tenth leading cause of death in the United States. Homicide is 18th, to give some perspective.
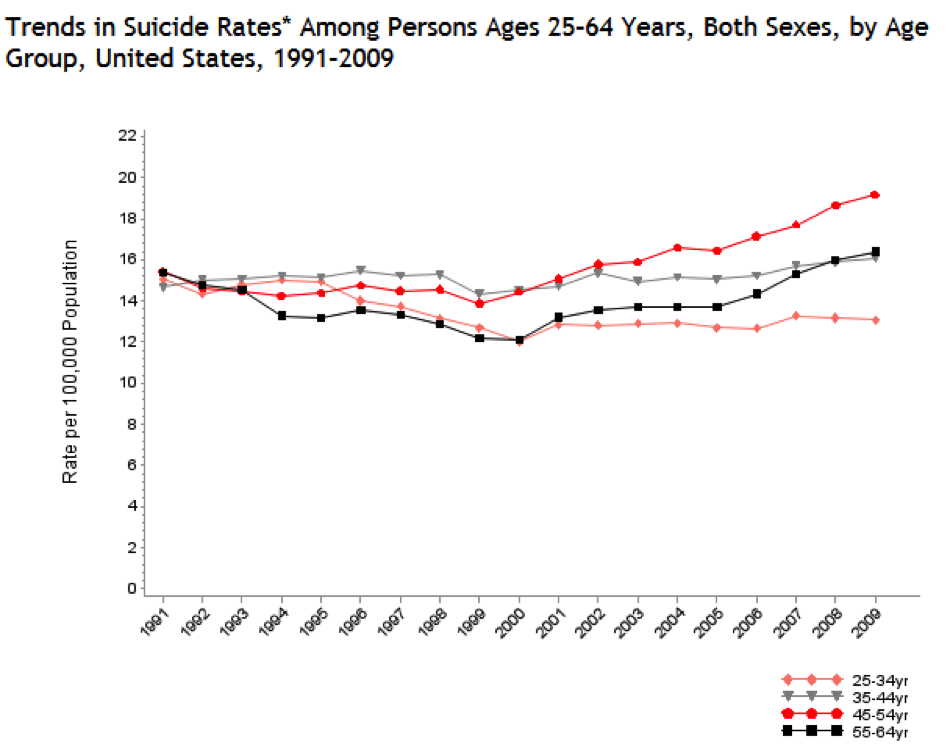
Completed may sound like a crude and technical term for such a tragedy, but it is used to highlight the fact that this statistic does not account for all the attempts made. A recent CDC report found that approximately 8.3 million adults (3.7% of the adult U.S. population) reported having serious thoughts of suicide in the past year. Suicide is the third leading cause of death among persons aged 15-24 years, the second among persons aged 25-34 years, and the fourth among person aged 35-54 years. Among individuals aged 45-54 years, the CDC reports that the suicide rate has increased 37.9% between 1999-2009.
Suicide does not occur out of the blue. It is precipitated by mental illness, a topic few in our purportedly enlightened society are keen to discuss. Perhaps the burden from mental and behavioral disorders, including depression and drug use disorders, would not have increased by 43% and 85% respectively from 1990-2010, had we broached this topic earlier. It is 2014 and Americans still cannot openly share their struggles with depression, anxiety or addiction. Instead, our society diverts opportunities for meaningful discussion about the burden of these chronic medical diagnoses by mislabeling them as stress.
According to the American Foundation for Suicide Prevention, 90% of individuals who complete suicide suffer from a potentially treatable mental disorder. Robin Williams did not commit suicide because of stress. He suffered from depression and addiction. He had also been recently diagnosed with early stage Parkinsons, a degenerative chronic illness that leads to loss of control of ones body, and likely contributed to his depression.
Most of us spend the majority of our time in two places; our workplace and our home. Both influence our mental well-being daily. The workplace provides the opportunity and has the responsibility to support Americans suffering from mental illness. If you accept that no workplace is free of employees struggling with stress, then you must come to terms with the fact that no workplace is free of employees struggling with mental illness. One in 10 Americans report current depression (in the previous two weeks) and 6.6% experience depression in the previous year. In a company with 100 employees this equals to 10 employees; in a company with 10,000 it translates to 1,000.
Major depressive disorder is one of the top 5 leading causes of disability in North America, Europe, Australasia, and much of Asia and Latin America. This burden is not unique to the United States; the entire world must use this terrible tragedy as a call to action. Businesses must lead the destigmatization of mental illness and promote mental well-being in workplaces and communities globally. High profile suicides have been followed by spikes in suicide rates in the past; therefore, responsible employers must reevaluate their workplace health promotion efforts today and ask the pressing question: Am I effectively addressing the mental and behavioral health issues of my workforce? We cannot risk carrying on about stress any longer.
Image Sources: CDC.gov and NBCBayArea.com.