Noncommunicable chronic diseases (NCDs) like cardiovascular disease and stroke, diabetes, and cancer are the main causes of mortality, morbidity, disability, and health care costs. At least half of these diseases can be prevented by modifying and reducing risky health risk factors such as tobacco use, physical inactivity, unhealthy diets, drug and alcohol abuse, and poor mental health.
In spite of this, national healthcare costs since the 1980s have been heavily skewed towards prescription drugs, medical devices, and clinical services, with public health and prevention activities consistently accounting for a meager 2%-3% of annual spending. The Institute of Medicine proposed that population burden of disease and preventability should be major determinants of priorities for public health interventions and the amount of research funding provided by the National Institutes of Health (NIH). The NIH is the worlds largest funder of biomedical research and receives 90% ($30 billion) of the $34 billion annual US federal health research and development budget. NIH funding priorities not only shape the nations scientific agenda, they also have a significant impact on funding for research universities and the career development of research scientists.
In a paper published in the American Journal of Preventive Medicine this week, we analyzed NIH funding trends for prevention between fiscal years 2010-2012 for human behavioral interventions that target the modifiable risk factors of six major and costly NCDs cancer, coronary heart disease, hypertension, stroked, diabetes and obesity. Our main findings include:
- Absolute funding for prevention has remained stable and substantially lower versus funding for biomedical treatments and cures (approximately 20% vs. 80%)
- The current prevention portfolio comprises approximately 63% basic biomedical, genetic and animal studies versus 37% for human behavioral studies
- The majority of funding for prevention comprised secondary prevention studies (65%) targeted at the individual-level (71%)
- Diet and exercise were the most studied risk factors (41%), and few studies conducted economic analyses (12%)
- NIH spends an estimated $2.2-$2.6 billion (7%-9% of the total $30 billion) on human behavioral interventions to prevent NCDs
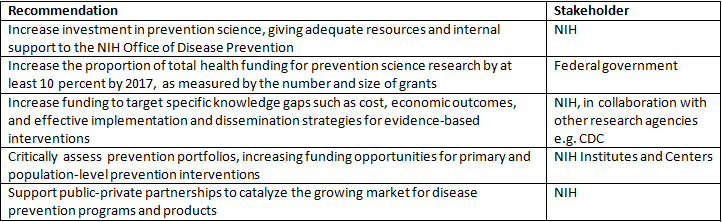
Current funding levels for prevention do not reflect the opportunities to improve population health through disease prevention and health promotion. For the US to improve its lagging performance on population health compared to other high-income countries, it is imperative to address several key issues related to federal funding for prevention and health promotion. Our recommendations include:
The shift in the disease burden profile in the US has profound implications for the types of resources and partnerships now needed to control the rapidly rising costs of NCDs. Investing in prevention, and prevention research and science, should be a strategic national priority to help improve the lagging population health of the US compared to other industrialized countries.
Source of image: Dr Proodian’s Blog